Stress Fractures In Active People
Unlike the more traumatic and painful fractures that result from falls or impacts, the more common STRESS fractures do not require the excitement of surgery, hospitalization, and painful rehabilitation. However, minor as a stress fracture may seem, it is a condition that will severely impact on your sports training and race plans for up to 3 months. Let me share some facts with you about stress fractures, and how to prevent them.

What’s a STRESS FRACTURE?
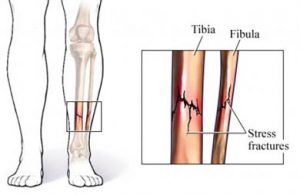
It’s an injury to one of your bones, usually the shin bone (tibia) or bones of your feet (metatarsal). Stress fractures may occur in other bones too, and for those who run, stress fractures of the pelvis and thigh bone need to be considered. The stress fracture is an actual crack in the bone that may be complete or incomplete. It is the severity of crack and the bone’s response to the injury that determines how much time needs to be given to allow the bone to be placed under the stress of exercise again.
What causes it?

When you run (and it is mainly running that causes the shin and foot stress fractures), your feet and leg bones are subjected to repeated impact and stress. The bone needs to time to repair any microscopic strain that has developed. When there is not enough time to heal, the bones develop progressive damage that finally results in the stress fracture.
The most common causes of this build-up of injury-causing stress are:
- A training program that has sudden increases in frequency, intensity or duration of your running
- Too rapid and sustained build-up of running mileage, not allowing proper periodisation recovery for the bones
- Change of running style without sufficient adaptation time
- Insufficient running shoe cushioning (eg. Using racing flats for most runs) or support (eg. If you have pronating or flat feet)
- Running on hard surfaces
What does it feel like?

Painful. The pain occurs at the site of the stress fracture. In the shin, this is most commonly at the place where many runners complain of having “shin splints”: along the inner lower shin. The pain occurs during runs, but stops with rest. As the stress injury gets worse, the pain comes on earlier in the run, does not stop immediately with rest, and may even persist the next day while walking. It may be painful to touch or press the area of pain on the shin bone.
How do I treat it?
With great respect!!! See your Sports Medicine doctor if you suspect you may have a stress fracture. Useful things to bring along include your running shoes (to check for shoes factors) as well as your training log or diary that includes the period leading up to the onset of pain. After reviewing you, the doctor may order a X-ray, bone scan, or MRI. X-rays may not show up bone injury or a fracture pattern for weeks after the stress fracture injury starts. Bone scans can be non-specific in what they show as an injury “hot spot.” And so it is the MRI that is increasingly used to not only show the bone damage, but the extent of it. This helps to indicate the likely healing time – in other words, the time you need to stay off running.
If I have a stress fracture, how do I keep on training?

Your Sports Doctor will be able to lay out an injury healing plan for you that includes continuing your physical training, albeit with a reduction in running. This may involve:
Stopping running and weight-bearing exercise for up to (gulp) 12 weeks (which may cause you heartache in addition to your stress fracture pain…)
Changing or replacing your running shoes
Using more cushioned footwear for everyday use, and when you resume running again
Use of arch supporting, cushioned insoles for your work and exercise shoes
Changing your training program over the immediate and longer term, involving how often, how long, and how far you run.
A longer term training periodisation plan
Continuing swimming (being careful with push-offs from the pool walls)
Continuing cycling (unless you have a metatarsal stress fracture) but staying in the saddle even when climbing to reduce stress through the leg and foot bones)
Deep water running using a flotation vest
Nutritional review (eg. of calcium sources in your diet).
Special emphasis on stress fractures in women triathletes

Hi there, ladies. Here’s something just for you. Sports Medicine books used to refer to something called the “female athlete triad.” This may be relevant to you if you have experienced or are experiencing what seems to be a delayed start of menstruation (for you younger triathletes) or if you are no longer having your periods (meaning that you have had menstrual periods, but with the progress of your training, your menses have stopped). Check in with your Sports Doctor if this might be an issue for you.
Written by Dr Low Wye Mun (Sports Medicine Consultant).
Pacific Healthcare Specialist Centre
www.sportzdoc.com
Tips* Asking questions is one of the best ways to ensure you and your doctor are on the same page.